Family care is a key part of hospital care, so let’s start talking about it that way.
Family care is a key part of hospital care, so let’s start talking about it that way.
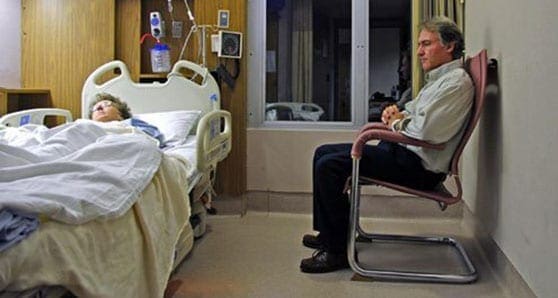
When a loved one is admitted to hospital, family caregivers want to offer comfort and support at the bedside. But in order to perform their healing role, they need to be recognized as key members of the hospital treatment team.
They’re keepers of their loved one’s medical history and they’re experts in their experience of illness, as well as in their personal tastes and preferences. Family caregivers represent the whole, well person to medical professionals who may only see an ill patient.
Natural caregivers perform a vital role in hospital and as care managers in the transition to home after discharge. Just because family care is borne of love and is unpaid, it shouldn’t be seen or represented by healthcare bodies as arbitrary and outside the patient treatment plan.
Family caregivers are an essential conduit between the patient and all hospital professionals. And they perform a good deal of personal care. They’re the purveyors of comfort and they’re personal valets. They deliver glasses of ice water, extra blankets and lots of gentle hugs.
The problem is that hospital administrators and clinical staff don’t often admit freely to the vital role that families play as partners in care. In fact, the messaging on hospital websites invites the public to believe families simply provide an antidote to the stress of acute illness and being away from home.
Here’s what one adult hospital wrote about visitors on its website: “We encourage you to visit your loved one at any time because we know that having family and friends nearby helps reduce anxiety and isolation.”
Even though nurses rely on families to provide assistance to patients, especially for frail seniors and people with disabilities or chronic illness, hospitals still charge anywhere between $14 and $25 per day for visitor parking – a cost that galls family members working at their loved one’s bedside all day, every day.
Dr. Samir Sinha, director of geriatrics at Mount Sinai Hospital in Toronto and expert lead of Ontario’s Seniors Strategy, is a passionate champion of seniors and their families as partners in care.
“Family caregivers are essential ‘must-haves’ for frail elders who find themselves either hospitalized or in an emergency department,” he reflects. “The absence of a family member to provide context about the patient can sometimes lead to misperceptions that encourage premature institutionalization or the risk of a poorly planned discharge home.”
At children’s hospitals, parents are encouraged to take part in their child’s care. This is the way one major pediatric hospital phrases the parental role on its website: “Parents are encouraged to take part in their child’s care. You may stay overnight and sleep on the sofa in your child’s room for the duration of their stay.”
The message is that parents are more than welcome to move in with their sick child. That shows just how central parents are in their child’s care while in hospital. The reality of pediatric care today is that nurses, doctors and therapists perform assessments and procedures, but it’s parents who soothe, monitor, distract and report on their child to staff, all day, every day.
Assistance with nearly all activities of daily living is up to families. This is particularly true for young children, and patients with disabilities or chronic impairments of any kind. Today’s wards are staffed based on caring for a sick but otherwise self-sufficient patient population. The reality is that the more dependent the patient, the more he or she needs a family caregiver in the hospital.
None of this is the fault of our country’s highly-trained and compassionate medical professionals. It’s simply an uncomfortable stage in the evolution of Canadian healthcare – caught between the old model of paternalistic systems and the contemporary reality of a population that’s living longer, but with more illness and earlier hospital discharges – all with families as the backstop.
Inviting family members to contribute to hospital charts, providing them with comfortable in-hospital accommodation including access to kitchen and shower facilities, and free hospital parking when their loved ones are patients are just a few ways hospitals can support the critical role of families in patients’ circle of care.
Donna is a Troy Media contributor. Why aren’t you?
The views, opinions and positions expressed by columnists and contributors are the author’s alone. They do not inherently or expressly reflect the views, opinions and/or positions of our publication.
An aging Canadian population and smaller families, combined with reduced health and social care budgets, mean the challenges of providing care to seniors will only worsen. Legions of families are buckling under the emotional, physical and fiscal burdens of caregiving. These pressures will be exacerbated by growing numbers of people living with demanding health challenges such as dementia, with fewer and fewer people to take care of them. The natural web of caring that so many of us take for granted is at risk of unravelling. Troy Media’s Family Ties examines the issues facing caregivers and the healthcare system in general and seeks solutions. If you have a story to tell, contact us at [email protected]. We would love to hear from you.