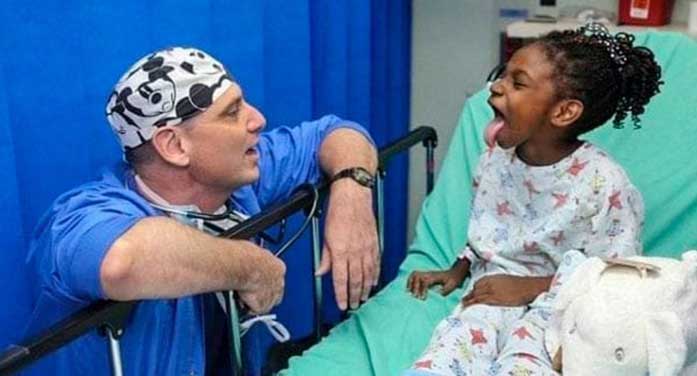
As a medical student at Toronto’s Hospital for Sick Children (SickKids), I saw first-hand the lives and healthcare needs of low-income families in Toronto. Seeing those families helped me recognize how societal factors affect their well-being.
As a medical student at Toronto’s Hospital for Sick Children (SickKids), I saw first-hand the lives and healthcare needs of low-income families in Toronto. Seeing those families helped me recognize how societal factors affect their well-being.
In the social paediatrics course I was taking, I worked to improve the health of children of young parents, in clinics with multi-disciplinary teams. There were times when I felt overwhelmed by the incredible number of obstacles these families face.
I met a teenage mother raising her baby in a shelter; I met a refugee who found creative ways to feed herself and her child on $200 a month after escaping an abusive relationship. I learned the source of significant weight loss for a very young teen mother was because her paycheque was used to feed her extended family, not herself.
The Toronto Children’s Aid Society recently published a report saying that 30 percent of children in Toronto are from low-income families. That means almost 146,000 children are growing up in low-income families in Toronto, facing higher risks for almost every kind of illness and disease.
When a doctor regularly meets patients who face poverty, food insecurity, lack of safe housing, and psychosocial stressors, it reinforces the necessity to ask about their social and living conditions.
We don’t know unless we ask. And we don’t ask unless we understand the reality of those living in poverty. I was reminded of this after meeting children and mothers who have experienced physical and emotional abuse, for example. And after meeting families who might not have insurance or access to government subsidies for medications, lotions or treatments. In these instances, asking questions regarding safety and income becomes paramount.
By the end of medical school, students should have a good understanding of what public health experts call the social determinants of health. I was reminded of this on a daily basis during this course.
I saw countless examples of strength and resilience as well as the power of acts of generosity. This may not be a part of the physiology we study, but it plays a significant role in health and healing. I realized why an understanding of the social conditions of our patients should shape our approach to health and healthcare.
But it can be a challenge for medical students and residents to translate our knowledge of the social determinants of health into our practice.
Medical schools teach a lot about patient-centered care. But there is a need for more exposure to the daily struggles of disadvantaged families. There is also a need to integrate patient advocacy into medicine in order to learn practical ways to create meaningful change.
This means providing treatment options that are feasible, affordable and practical for families. It requires insight into food and housing insecurity and how poverty may manifest as illness or present challenges to adhere to treatment.
My time at SickKids also gave me some insight into the dedication of community organizations and allied health professionals in addressing unmet needs on individual, community and policy levels.
I wish more of my fellow medical students could share this experience. Being immersed in a culture of medical practice where a deep understanding of the experiences of marginalized groups influences not only the questions asked, but also the treatment strategy and approach.
Many of my peers in social paediatrics have helped me understand a doctor’s role as an advocate – how to address injustice within the healthcare system and ways to design a medical practice to see health beyond illness. Social determinants of health are no longer an abstract concept.
Lita Cameron is a Family Medicine resident at McMaster University. She completed her Masters in Global Health Science at Oxford University. This article was prepared in consultation with Elizabeth Lee-Ford Jones professor of Paediatrics at The Hospital for Sick Children and the University of Toronto.
Lita and Elizabeth are Troy Media contributors. Why aren’t you?
The views, opinions and positions expressed by columnists and contributors are the author’s alone. They do not inherently or expressly reflect the views, opinions and/or positions of our publication.